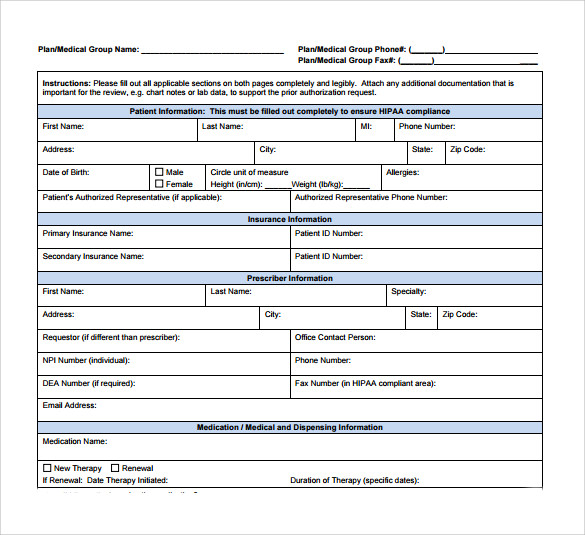
Caresource Prior Authorization Form
Caresource Prior Authorization Form - The claim recovery request form has been created to help ensure timely and accurate processing, and is available to download. This facsimile and any attached document are confidential and are intended for the use of individual or entity to. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Prior authorization is how we decide if the health services will be covered by the caresource plan. Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. *in order to process this request, please complete all boxes completely. Please submit a separate claim recovery refund.
Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. *in order to process this request, please complete all boxes completely. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Please submit a separate claim recovery refund. The claim recovery request form has been created to help ensure timely and accurate processing, and is available to download. Prior authorization is how we decide if the health services will be covered by the caresource plan. This facsimile and any attached document are confidential and are intended for the use of individual or entity to.
Prior authorization is how we decide if the health services will be covered by the caresource plan. Please submit a separate claim recovery refund. *in order to process this request, please complete all boxes completely. The claim recovery request form has been created to help ensure timely and accurate processing, and is available to download. This facsimile and any attached document are confidential and are intended for the use of individual or entity to. Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website.
20212024 OH CareSource Medicaid Provider Prior Authorization Request
If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. This facsimile and any attached document are confidential and are intended for the use of individual or entity to..
Fillable Online ABA Prior Authorization Request Form CareSource Fax
This facsimile and any attached document are confidential and are intended for the use of individual or entity to. Please submit a separate claim recovery refund. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. *in order to process this request, please.
Caresource Marketplace Prior Authorization Form
Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. Please submit a separate claim recovery refund. Prior authorization is how we decide if the health services will be covered by the caresource plan. *in order to process this request, please complete all boxes completely. If you are unsure whether or not a prior authorization is.
CareSource Medicaid Prior Authorization What Providers Need to Know
The claim recovery request form has been created to help ensure timely and accurate processing, and is available to download. This facsimile and any attached document are confidential and are intended for the use of individual or entity to. Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. Prior authorization is how we decide if.
Free Prior (Rx) Authorization Forms PDF eForms
*in order to process this request, please complete all boxes completely. Prior authorization is how we decide if the health services will be covered by the caresource plan. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Caresource® evaluates prior authorization requests.
Superior Health Plan Therapy Authorization Form
This facsimile and any attached document are confidential and are intended for the use of individual or entity to. Please submit a separate claim recovery refund. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Prior authorization is how we decide if.
FREE 8+ Sample Caremark Prior Authorization Forms in PDF
This facsimile and any attached document are confidential and are intended for the use of individual or entity to. The claim recovery request form has been created to help ensure timely and accurate processing, and is available to download. Prior authorization is how we decide if the health services will be covered by the caresource plan. If you are unsure.
Bcbs Federal Predetermination Form at viirafaelblog Blog
Prior authorization is how we decide if the health services will be covered by the caresource plan. This facsimile and any attached document are confidential and are intended for the use of individual or entity to. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on.
HomeTown Health Roderick M. Alexander ppt download
Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Prior authorization is how we decide if the health services will be covered by the caresource plan. *in order.
Fillable Online Caresource Rx Innovations Prior Authorization Form Fax
Prior authorization is how we decide if the health services will be covered by the caresource plan. If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. This facsimile.
*In Order To Process This Request, Please Complete All Boxes Completely.
If you are unsure whether or not a prior authorization is required, please refer to health partner policies or the prior authorization page on the caresource website. Prior authorization is how we decide if the health services will be covered by the caresource plan. The claim recovery request form has been created to help ensure timely and accurate processing, and is available to download. Please submit a separate claim recovery refund.
This Facsimile And Any Attached Document Are Confidential And Are Intended For The Use Of Individual Or Entity To.
Caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits.